Click here to check Jane’s Pilates Classes availability
My thoughts on Osteoporosis and Exercise
Since I started teaching Pilates I have become increasingly interested in learning more in order to support those with back conditions. I have therefore attended training courses over the last year, which cover back care and – specifically – osteoporosis, as I currently work on a one-to-one basis with several clients who have osteoporosis. There are also many people with back conditions who attend my regular classes, and who therefore need to know what they should and should not be doing in order to strengthen and support their backs. Osteoporosis and Exercise should go hand in hand!
In this article, I share some of this information on osteoporosis and exercise, along with some of my experiences working with those who have back problems. This article is for those with little prior knowledge about osteoporosis. It will cover the risk factors, and how we can reduce these to help maintain our bone density.
I find that more physiotherapists and doctors are referring their patients to attend Pilates classes. This is great because of the benefits that Pilates offers us all in improving posture, core stretch and improved flexibility. A problem arises though, if the Pilates instructor does not have the necessary knowledge to offer suitable alternatives to help people with a back problems.
As well as being my passion, I see it as my responsibility to keep as many people mobile and active for as long as possible as they get older. I am overwhelmed by how many of my participants who have had back pain come to me after even just one session and say their back pain has reduced or gone, and that they are sleeping pain free. In my 27 years of teaching fitness classes, no other form of exercise has had those kind of results.
Learn more about my One to One Pilates Sessions
What is osteoporosis and who can get it?
Osteoporosis is the weakening of our bones due to a reduction in their density, or more scientifically: a systemic skeletal disorder characterised by low bone mass and micro-architectural deteriorations of the bone tissue with consequent increase in done fragility and susceptibility to fracture (Consensus Department Conference, 1993).
One in two women and one in five men over the age of 50 experience fractures, mostly as a result of low bone strength. Although fragility fractures caused by osteoporosis can happen in various parts of the body, the wrists, hips and spine are the most commonly affected sites (National Osteoporosis Society, 2016).
- 536,000 osteoporotic fractures occur in the UK annually.
- Within a year of a hip fracture, 33% of patients remain dependent or require nursing home care, and up to 24% will die.
Women are more susceptible to osteoporosis due to the menopause and an increase in bone loss for several years after this. This is due to sex hormone levels decreasing. Women have smaller bones, and in general live longer than men.
Men can also get osteoporosis (one in five men over 50 break a bone due to low bone strength. Men can sometime struggle with accepting they have osteoporosis, and are therefore less likely to seek help.
Younger men and women can sometimes be affected by osteoporosis. It is more unusual and often there is an underlying condition or reason. Research shows that if young adults exercise their bone density will be higher than those who do not.
Osteoporosis risk factors?
- Genes: family history, previous or parental history of hip fractures.
- Age: being over 50 years old.
- Gender: osteoporosis is more common in women because they have smaller bones and loss oestrogen during menopause.
- Race: Caucasian or Asian origin have a higher risk.
- Low Body Mass Index (BMI) : less than 19 – low body weight.
- Unhealthy lifestyle: low physical activity, smoking, excessive alcohol, lack of calcium and vitamin D.
- Certain medications: such as steroids and some treatments for Crohn’s disease.
How do you know you have Osteoporosis?
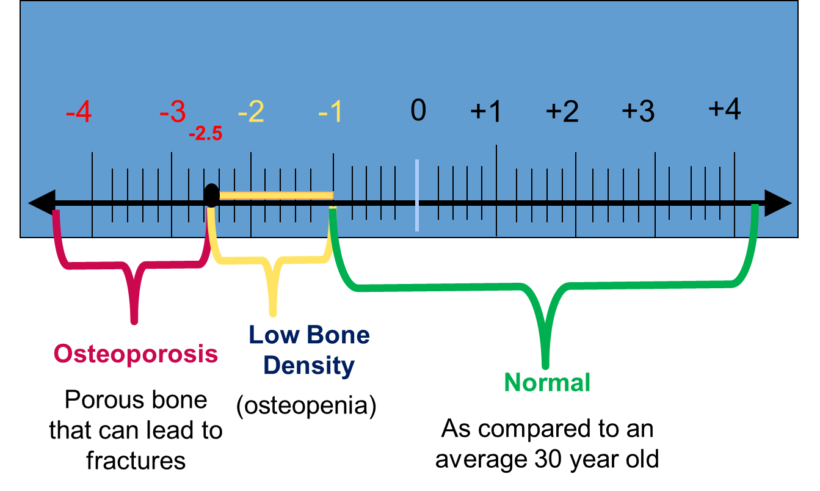
Bone density can be measured according to a scale known as the T-score. Below are the T-score ranges for normal bones, osteopenia and osteoporosis.
A T-score of -1 and above is normal. -1.0 to -2.5 signifies osteopenia, meaning below normal bone density without full-blown osteoporosis. This stage of bone loss is the precursor to osteoporosis, which corresponds to a T-score of -2.5 and below.
What you can do to help yourself
- Take regular exercise: 30 minutes of moderate intensity physical activity at least 5 times a week (150 minutes in total). Older adults (over 65) should add balance and co-ordination at least twice a week.
- Eat the right foods and ensure adequate calcium and vitamin D intake.
- Aim for a healthy weight.
- Reduce or cut out fizzy drinks.
- Reduce your amount of alcohol consumption, as excess alcohol appears to slow down the bone renewal process.
Healthy eating for your bones
We all need to maintain a healthy lifestyle with regard to eating and drinking. This shouldn’t just start when we are diagnosed with osteoporosis, but continue all the way through our lives, in order to maintain the correct nutrients, vitamins and minerals for good health. I shall cover two of the key minerals/vitamins for this article. The National Osteoporosis Society go into much more detail and it is worth reading their full article on Food Facts and Bones.
Calcium is needed for our teeth and bones. 700mg of calcium is sufficient as an adult daily requirement. Foods higher in calcium are cheese, milk (including soya milk), tofu, sardines, and salmon. There are many other foods which contain calcium. There are many vegetables such as green beans, cabbage, broccoli, watercress, onions and tomatoes which contain calcium.
Vitamin D is needed to help regulate the way our bodies use calcium, and to ensure your bones, muscles and teeth remain strong. Vitamin D can be produced by the skin when it is exposed to sunlight. It may also be found in foods such as fatty fish (e.g. tuna, mackerel, and salmon), some dairy products, orange juice, soy milk, cereals, beef liver, cheese and egg yolks.
Osteoporosis and Exercise – should I?
Yes! As I said at the start, osteoporosis and exercise should go hand in hand. Chose weight bearing exercise, which is any exercise whereby you are supporting your own body weight through your feet and legs, or hands and arms. The key is to remain active and find something you enjoy. This could be walking every day, dancing, cycling, aqua aerobics using resistance equipment, or Pilates.
What exercises should I avoid if I have Osteoporosis?
Avoid exercise which involves impact or falling. Sports such as horse-riding and skiing have a higher risk of falling and possible fractures. Long distance running on a treadmill can cause fractures over time due to the constant impact.
Exercises to avoid will vary depending on the severity of Osteoporosis, and the fitness of the person. Discuss this with your instructor prior to taking part in exercise. Some examples of exercises to avoid include
- Using a foam roller (rolling off could cause problems).
- Neck hyper-extension (lifting the head backwards towards the spine).
- Forward flexion and rotation: no roll down with a twist (touching your toes and then twisting at the same time).
- Roll back or roll over backwards (in a ball rolling back on the spine).
- Fixed rotation such as: saw and oblique twists (twisting of the upper body too much).
- Thoracic flexion such as curl ups.
- Shoulder stands and anything which puts pressure on the back of the neck.
What exercises should I be doing if I have Osteoporosis?
Note: always check with your instructor if you are not sure or have any questions.
Strength training and weight bearing exercise. Strengthen the key core muscles, the wrists, shoulders, hips and spine. Use weights and resistance bands to strengthen the arms, back shoulders and wrists. Balance work is important to improve stability, but also to increase weight bearing on the legs to strengthen them. Lunges, squats and step ups are also good to strengthen the legs. Limited impact work such as jumping can be completed for short periods of time in the earlier stages of osteoporosis.
Pilates for Osteoporosis
Join one of my local Pilates classes
Osteoporosis and exercise should go together, but for effectiveness and safety, it must be the right type. Pilates is an excellent form of exercise for people with osteoporosis, as individual exercises can be performed at many different levels of intensity, enabling people to progress in a controlled manner and at their own pace. The weight bearing, balance and core stability elements of Pilates are especially helpful to people with osteoporosis.
Good technique is important to keep the back in alignment; this is especially important for people with osteoporosis. Correct technique when squatting, and also when getting up and down off the floor is very important. Avoid bending and stooping. Instead keep the back straight and use the legs to support the movement. In order to complete the above moves correctly the core muscles need to be engaged as well as the legs.
Balance work is a great way to improve stability, and one legged standing is also more weight bearing than standing on both feet. This helps to work the stabilisers in the legs and the core muscles of the middle (Transverse Abdominis (TVA) to hold the position. This will have 3 benefits:
- Lessens the likelihood of falling.
- Strengthens the muscles.
- Improves confidence to keep active and mobile.
There are several exercises on the mat which will help strengthen the abdominals, plus the arms and legs. These are also weight bearing for the arms and hips. The good old plank is a great example. Planking primarily strengthens the TVA, but also the wrists if completed on the hands, plus the shoulders are also working to hold the position. This can be done in a box position, three quarter or full plank, depending on your fitness. It can also be performed on the elbows if the hands are too weak. There is always a harder lever to progress to over time! (The plank can also be completed against a wall if you are not able to go to the floor.)
If you would like more information on other exercises, osteoporosis and exercise, as well as an individual posture analysis, please do get in touch with me. I have already helped many of my 1:1 clients with osteoporosis improve their quality of life, and want to help more people learn how to live with this condition and keep active and healthy.
Contact Jane Mackenzie for more information
Useful links for additional reading
- National Osteoporosis Foundation
- National Institute for Aging
- National Osteoporosis Society
- Publications which can be downloaded
Click here to check Jane’s Pilates Classes availability
 Jane on WhatsApp
Jane on WhatsApp